ddxof: POCUS for Undifferentiated Shortness of Breath
Undifferentiated Shortness of Breath
This is a co-post with our FOAMEd partner The ddxof - project of Dr. Tom Fadial . ddxof: is a compilation of cases based on real patients, each inspiring an algorithm for the evaluation and management of their chief complaint or diagnosis.
If you have any ideas for collaborating with our team don't hesitate to reach out.
Please see the original post here https://ddxof.com/ultrasound-in-dyspnea/
This is a common emergency department scenario: a critically-ill patient with undifferentiated dyspnea. The physical exam can be difficult and indeterminate with huge risks of deterioration. Our CHF patients often have COPD, afib and maybe renal failure. Your decisions matter. Here is a proposed approach for these patients.
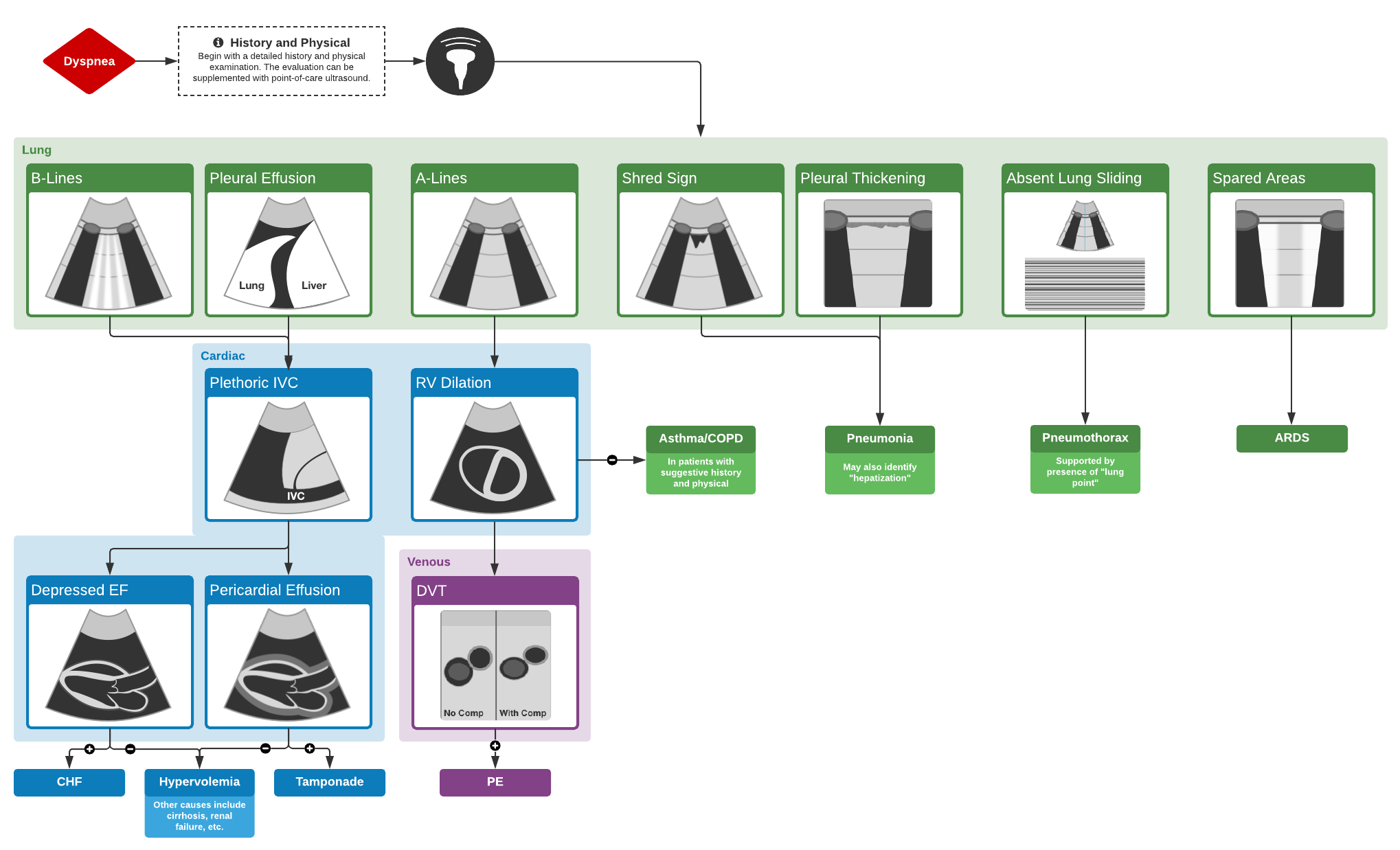
Algorithm for the Use of Ultrasound in the Evaluation of Dyspnea
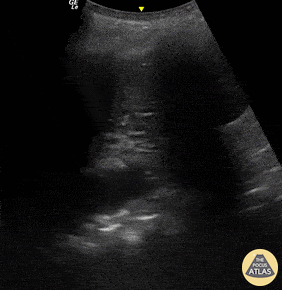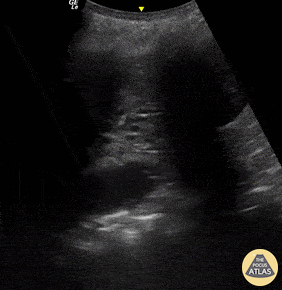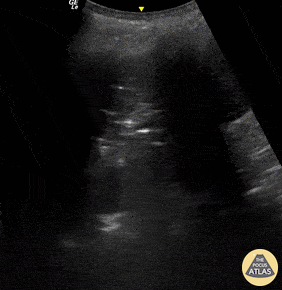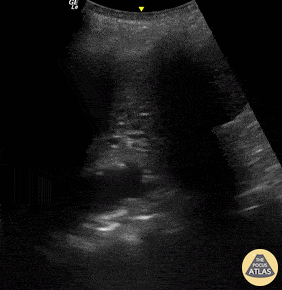
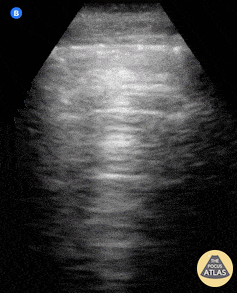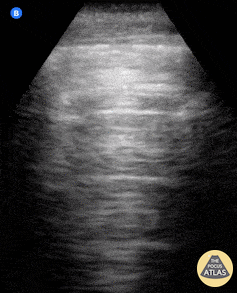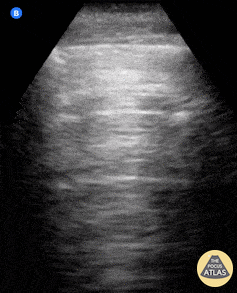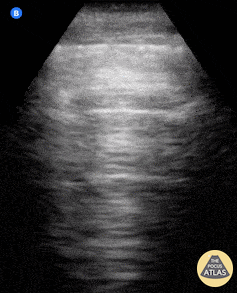
Seen here is an irregular and thickened pleural line with associated focal and confluent B lines in a patient with COVID-19 pneumonia.
Edgar Miranda
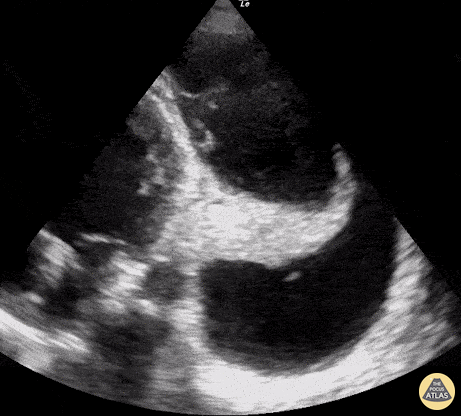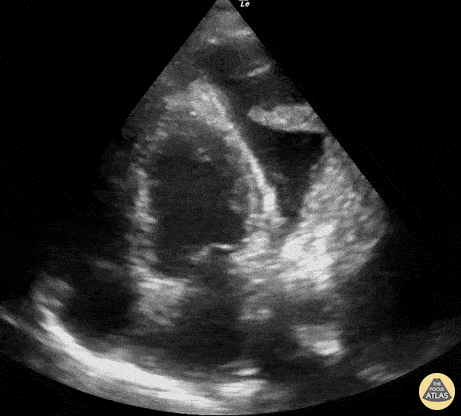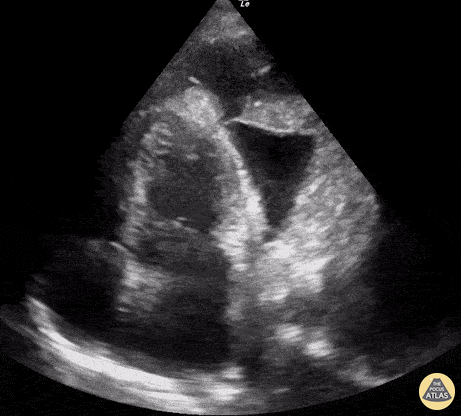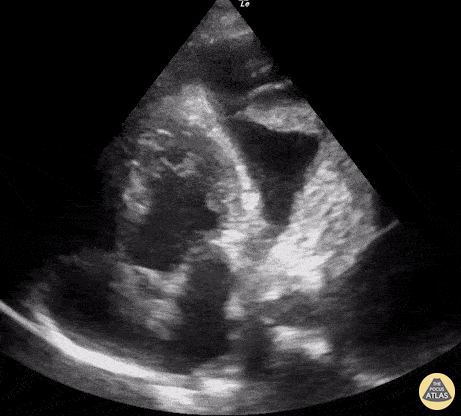
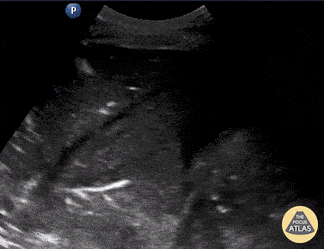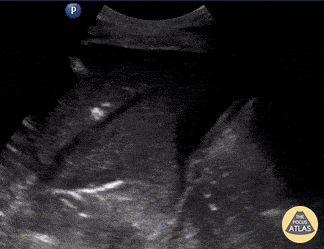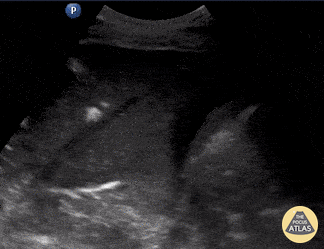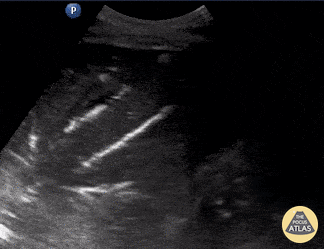
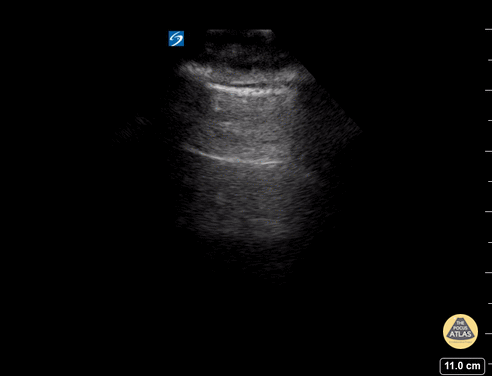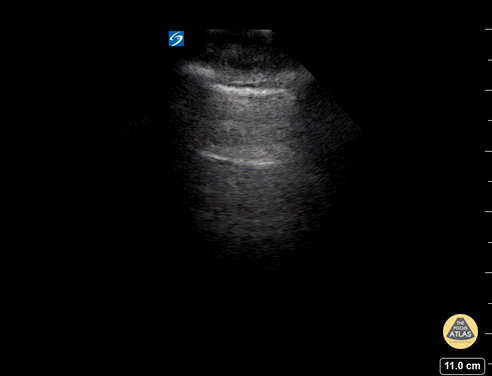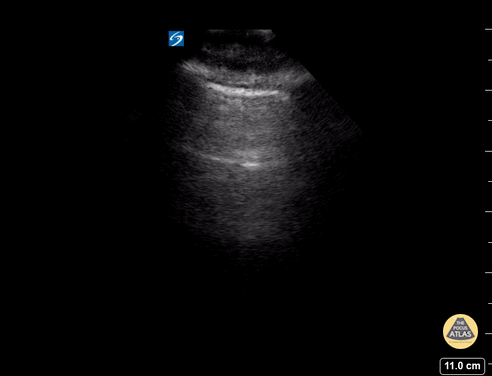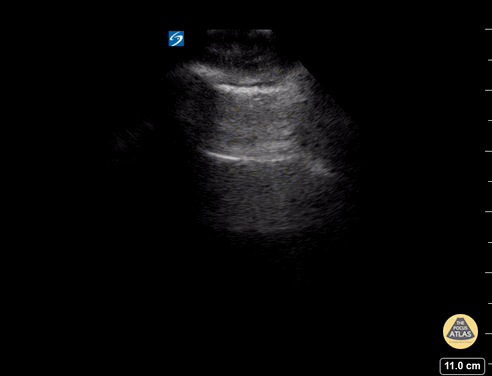
Seen here is an unexpected finding while acquiring an apical 4 chamber view with a phased array probe. The four chambers of the heart are difficult to bring into view due to the presence of large left pleural effusion with ipsilateral collapsed lung floating within the pleural fluid. This visual of atelectatic lung swimming within a pleural effusion is referred to as “jellyfish sign”.
Renato Tambelli, Emergency Physician Hospital das Clínicas de Marília, Brazil.
@R_Tambelli // @JediPocus
Pictured here are dynamic air bronchograms in a patient with bacterial pneumonia. Image was acquired using convex probe on the left PLAPS.
Renato Melo, PocusJedi co-founder, Emergency Physician HC Marília-SP, Brazil.
@Renato_Melo_
A 23-year-old male was admitted to the ED following a motorcycle accident. He subjectively reported dyspnea; objectively was hypoxic. POCUS seen here (obtained from L3 zone using curvilinear probe) reveals multifocal B-lines consistent with pulmonary contusion. This case illustrates that bedside US is useful beyond diagnosing pneumothorax and hemothorax in trauma patients.
Renato Tambelli, Emergency Physician Hospital das Clínicas de Marília, Brazil.
@R_Tambelli / @JediPocus
Patient presented with septic shock. POCUS was used to assess for etiology in this hemodynamically unstable patient. Shown here is a lung US windows (patients LLL) revealing a consolidation pattern with echoginicity similar to liver, referred to as “hepatization” of the lung. These findings are consistent with a diagnosis of pneumonia.
Johannes Achenbach
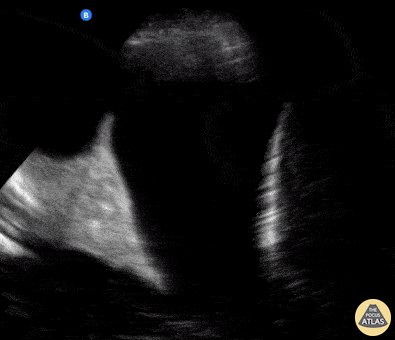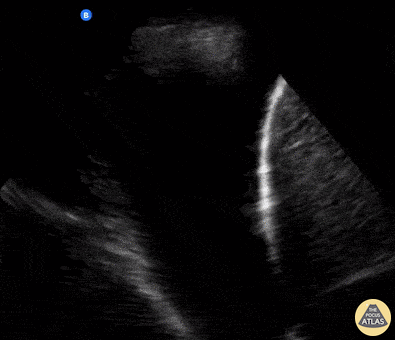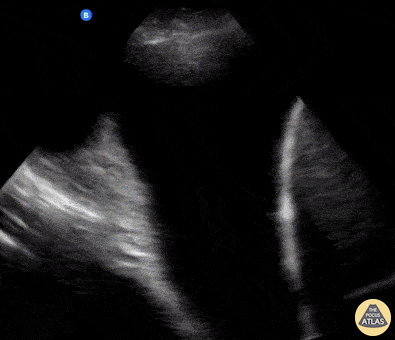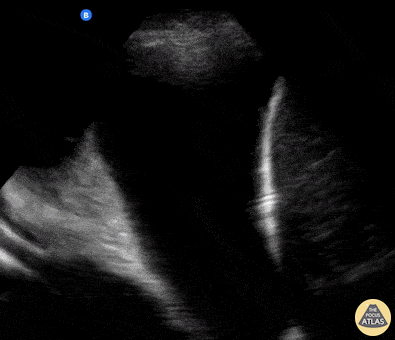
A middle age man presented with a subacute dyspnea, orthopnea, non productive cough, and paroxysmal nocturnal dyspnea. Physical exam was notable for bilateral, fine, end-inspiratory crackles over the lung bases; an S3 on cardiac auscultation; and an SpO2 of 92% on 2L nasal cannula.
POCUS identified the presence of atelectatic lung in an anechoic large right-sided pleural effusion. The sonographic appearance of atelectatic lung "swimming" within a large pleural effusion is often referred to as “jellyfish sign”. Subsequent laboratory evaluation of the pleural fluid confirmed a transudative effusion secondary to decompensated left-sided heart failure.
Al Chalaby, Shahad. PGY3. Highland Hospital. Alameda Health System Internal Medicine Residency Program.
@shahad_Chalaby
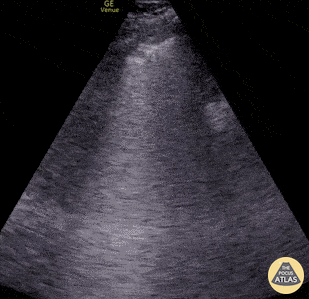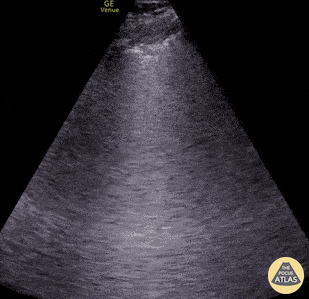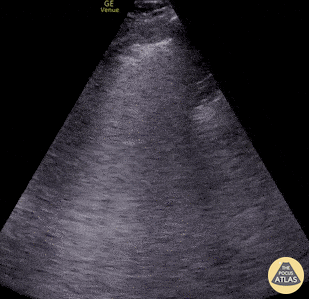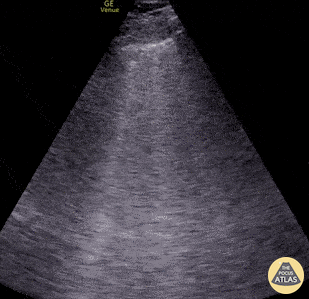
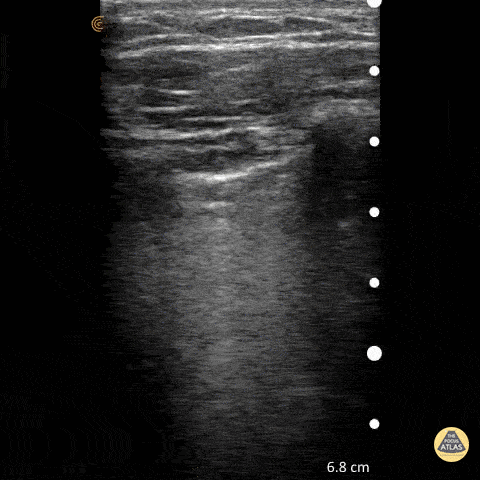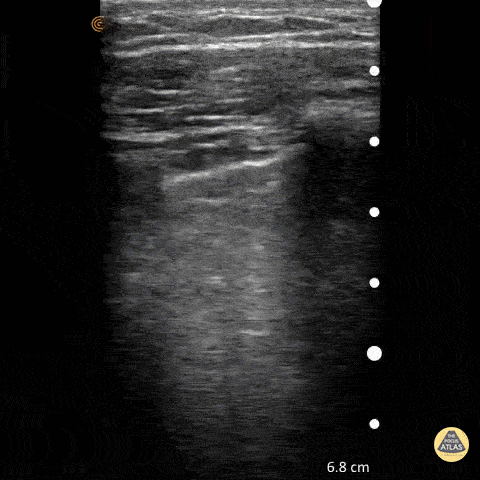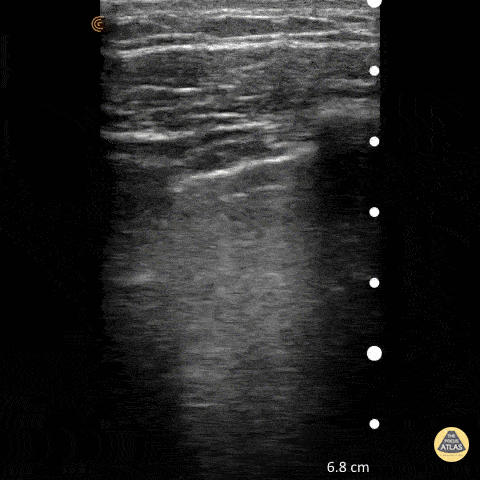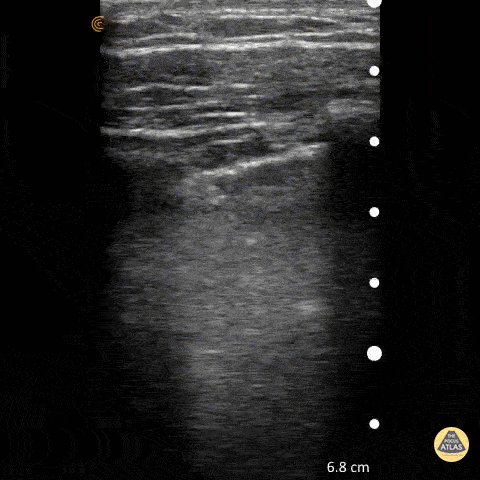
To assess for lung slide, look between two ribs. The two layers of pleura can be seen as the hyperechoic, shimmering line just under the subcutaneous tissue. This represents the sliding of the parietal and visceral pleura.
Normal lung slide should have: Shimmering aka "ants marching"
This may be augmented by m-mode as pictured in another post.
Dr. Matthew Riscinti - Kings County Emergency Medicine
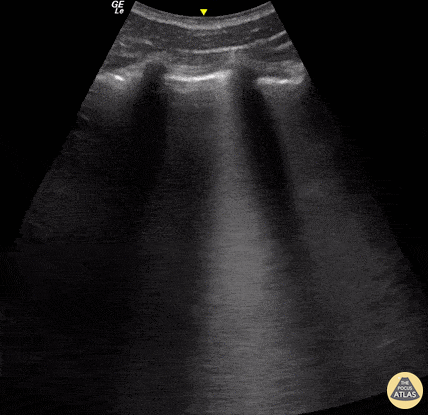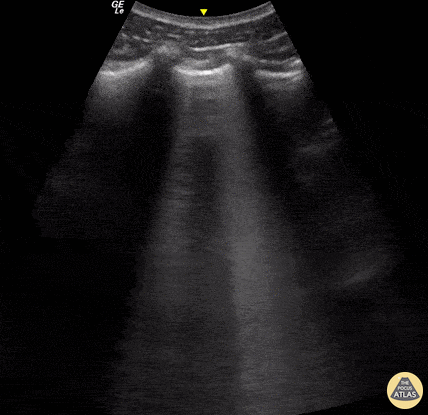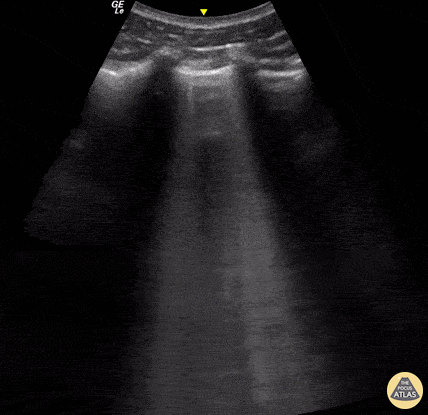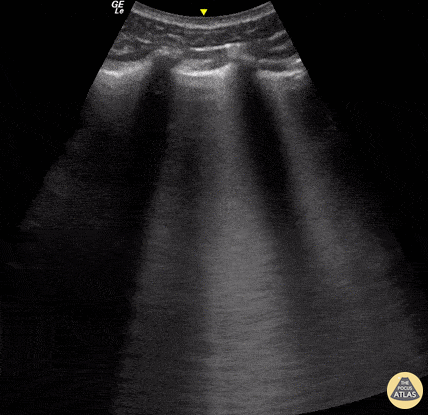
A lines appear as horizontal lines that represent normal aerated lung (dry interlobular septa). They are a reverberation artifact caused by the sound waves bouncing off the highly echogenic pleura and back to the probe, and repeating.
Hannah Kopinski (MS4) and Dr. Lindsay Davis - NYU Emergency Medicine, Matthew Riscinti - Kings County Emergency Medicine
Lung ultrasound of a normal lung. Note both lung slide (shimmery, hyperechoic line on top of the screen, a result of parietal and visceral pleura sliding against each other) as well as multiple parallel A-lines (normal artifact from reverberation of the pleural line). The presence of lung sliding and no more than 3 B lines on lung ultrasound help exclude inersitital pulmonary edema and pneumothorax.
Shahad Al Chalaby, MD. PGY-2, Internal Medicine
Highland Hospital, Alameda Health System Internal Medicine Residency Program. CA, USA
@shahad_Chalaby
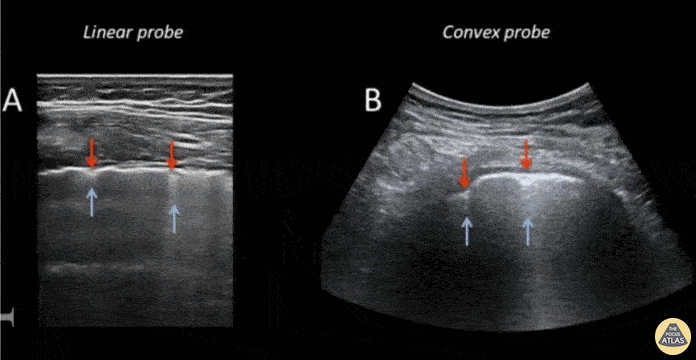
This still-shot image captures the differences in view as obtained using a linear vs curvilinear to assess a lung window.
Submitted by Anibal Artero
@ECOPULMONAR